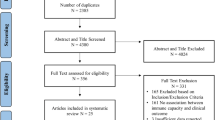
Abstract
Objective
Primary events such as severe injury and elective surgery cause a deterioration of the immune response measurable by reduction of expression of HLA-DR on monocytes or ex vivo LPS-induced TNFα production. The further influence of secondary surgery after severe injury on the immune response remains unresolved.
Design
Prospective observation study.
Setting
Surgical intensive care unit of an university hospital.
Patients
Sixteen severely injured patients with an ISS >25 points.
Measurements and results
On day 1 after trauma and immediately before secondary surgery, mean fluorescence intensity (MFI) of HLA-DR expression on monocytes and TNFα ex vivo synthesis was significantly reduced compared to healthy donors. Overall, surgical intervention during the second week after trauma caused no further reduction of HLA-DR expression on monocytes and of the ex vivo TNFα-synthesis. However, major surgery such as intramedullary nailing or pelvic osteosynthesis caused reduction of the HLA-DR expression and TNFα-synthesis, whereas, minor surgical interventions such as osteosynthesis on peripheral joints exhibited no significant effects on the immune response. Surgical intervention performed to clear septic foci normalised immune response by elevating HLA-DR expression on monocytes and ex vivo TNFα synthesis. Severe injury caused elevated serum IL-10 levels, whereas secondary surgery did not induce a further increase in serum IL-10 levels.
Conclusion
This study shows that initial trauma as well as major secondary surgery causes a suppression of immune functions, whereas minor secondary surgery does not cause significant immune disturbance.
Similar content being viewed by others
Introduction
Severe injury causes immune alterations with disturbed cellular and humeral immune response marked by a rapid decrease of human leukocyte antigen (HLA)-DR expression on monocyte as well as B- and T-cells [1, 2, 3]. The synthesis of cytokines such as tumour necrosis factor α (TNFα) or interleukin-6 (IL-6) after ex vivo lipopolysaccharide (LPS) stimulation is also down-modulated early after trauma [3, 4, 5]. Possibly, the anti-inflammatory effects of the cytokine interleukin-10 (IL-10) contribute to the downregulation of several immune functions after trauma, since this factor has been shown to be elevated after trauma [6]. In addition, IL-10 has been identified as factor decreasing HLA-DR surface expression on monocytes in patients with sepsis [7]. This hyporesponsiveness of the immune system after severe injury renders the traumatised patients susceptible to infectious challenges.
Surgical trauma causes similar changes of the immune response to those observed after accidental injury. Thus, decreased HLA-DR expression on monocytes have been observed after elective neurosurgery [8], cardiac surgery with cardiopulmonary bypass [9], after conventional but not laparoscopic cholecystectomy [10], and partial colectomy [11]. Surgical interventions, therefore, represent an additional challenge for the immune system that can superimpose on the trauma-induced disturbance of the immune response. Several studies demonstrated an inflammatory response caused by surgical trauma marked by elevated serum IL-6 and C-reactive protein (CRP) levels with a correlation between the degree of injury and the amount of circulating IL-6 [11, 12, 13].
The timing of secondary surgery after multiple injury can influence the incidence of multiple organ failure after trauma. A retrospective analysis of more than 4,000 severely injured patients revealed a higher incidence of multiple organ failure in patients sustained to surgery during day 2 and 4 than those with surgery after the 6th day following trauma [14]. Multiply injured patients operated on during a period of increased inflammatory response developed postoperative organ dysfunction more often than those with a normal homeostasis, as has been shown in a prospective study using CRP, elastase of polymorphonuclear granulocytes (PMN), and platelet counts as markers for the inflammatory response [14]. The role of secondary surgery after trauma as an additional burden on the immune system has been discussed in this and other papers. However, cellular immune functions after primary compared to secondary surgery after trauma have not been analysed in more detail yet. The treatment regime in the present study hospital consists of a primary damage control surgery and a definitive fracture stabilisation in the second or third week after trauma. The status of the immune response at the time of surgery and the impact of surgical intervention on the immune response in this phase after trauma have not been investigated. Therefore, in the present study we analysed HLA-DR expression on monocytes and ex vivo TNFα synthesis of blood cultures after trauma and after secondary surgery in multiply injured patients.
Material and Methods
Patients
This is a prospective study of severely injured patients with an Injury Severity Score (ISS) greater than 25 points, excluding predominantly blunt brain injury. The study group consisted of 16 consecutive patients with severe trauma admitted to the University Hospital of Essen, Department of Trauma Surgery, immediately after accident. Criteria for inclusion of patients were age (>18 and <80 years); ISS >25 points, and primary admission to the surgical intensive care unit within 8 h after accident. The specific threshold for the ISS was chosen, because a significant increase of posttraumatic multiple organ failure has been reported in patients with this degree of injury [15]. All of the patients’ medical histories were free of pre-existing immunological disorders, systemic steroid medication or known cancer disease. Sepsis was defined according to the consensus conference criteria published by Bone et al. [16]. Organ failure was evaluated on a daily basis applying the Sepsis-related Organ Failure assessment (SOFA)-Score [17]. Multiple organ failure (MOF) was defined as SOFA-Score >2 points of two organ systems persisting for more than 2 days. Blood from 12 healthy volunteers were collected at 0800 hours. The study and the additional blood sampling were approved by the ethic committee of the university of Essen, Germany.
Treatment protocol/surgical management
All patients received standardised emergency room management and intensive care treatment. After admission primary surgery was performed in the case of uncontrollable haemorrhage and for stabilisation of unstable fractures which was usually managed by external fixation. Spine injury were only primarily operated in the case of progressive neurologic deficit. As part of the general management at the study hospital definitive internal fracture stabilisation or plastic reconstruction were performed when platelet counts were above 80,000/mm3, CRP below 11 mg/dl or decreasing more than 20% within 2 days, and not more than one organ system with an SOFA-Score above 2 points, which was generally not the case before the 7th day after trauma. Almost all patients at the time point of surgery met these criteria except those with surgical focus clearance.
Classification of surgical interventions
Three different types of operation were defined: surgical intervention with the aim of clearing a septic focus (n=5), operation associated with a minor surgical trauma, such as osteosynthesis of peripheral joint fractures, secondary wound closures (n=9), and major surgery such as unreamed intramedullary nailing of long bone fractures or osteosynthesis of pelvic girdle and spine fractures (n=10).
Blood sampling
Arterial blood (heparinised blood samples, Sarstedt 5 ml and 10 ml heparin monovettes) was collected on the first day after hospital admission (day 1) and every Monday and Thursday after the accident at 08.00 hours until discharge from the intensive care unit. At the same time points serum was collected and stored at –20 °C until cytokine detection.
Whole blood stimulation
One millilitre of whole blood was diluted 1:1 with 1 ml RPMI 1640 medium containing 100 U/ml penicillin, and 100 µg/ml streptomycin, and glutamine and incubated in 12-well flat bottom tissue culture plates at 37 °C in an atmosphere of 5% CO2 in air. Blood cultures were set up as duplicates and incubated with 10 ng/ml lipopolysaccharide (LPS from Salmonella friedenau, kindly provided by H. Brade, Borstel, Germany) for 14 h before supernatants were collected after centrifugation for TNFα detection by means of enzyme-linked immunosorbent (ELISA).
ELISA
One hundred microlitres of the supernatant were used in the ELISA for TNFα detection. TNFα was determined using an ELISA purchased from Beckmann Coulter Company (Marseille, France). The lower detection limit was 15 pg/ml. IL-10 was detected in serum samples by means of ELISA. One hundred microlitres of serum sample were used for each detection. Each sample was analysed as duplicate. A commercially available ELISA from Beckmann Coulter Company (Marseille, France) was applied. The lower detection limit was 7.8 pg/ml.
Flow cytometry
In separate heparinised blood samples phenotyping of leukocytes was conducted by two-colour flow cytometry using whole blood lysis technique and monoclonal antibodies. Antibodies used were: phyctoerythrin conjugated (PE) CD14, FITC coupled CD45, and HLA-DR, PE/FITC conjugated paired isotype control antibodies (all antibodies Becton Dickinson, Heidelberg, Germany). To 20 µl of antibody pairs 100 µl of heparinised blood was added and incubated for 20 min. The erythrocytes were lysed with 2 ml FACS lysing solution (Becton Dickinson, Heidelberg, Germany), centrifuged, and washed twice with 2 ml PBS. Measurement of stained cells was performed with a FACscan (Becton Dickinson) counting 20,000 cells for each measurement. Flow cytometry defined the monocyte population using scatter characteristics and CD45/CD14 fluorescence staining. This monocyte population was analysed for HLA-DR expression, which is expressed on all monocytes. Flow cytometric analysis was conducted using a linear format to measure channel fluorescence intensities as numerals and to calculate mean fluorescence intensity (MFI) values. Paired isotype controls were run with each samples revealing always less than 2% unspecific binding. Ten thousand cells were computed in list mode and analysed using the FACScan research software (Becton Dickinson, Heidelberg, Germany). The results are expressed as HLA-DR molecules on the cell surface of monocytes, given as MFI-values.
Statistics
Values are expressed as boxplots with representation of median, 75th and 90th percentile or as mean±standard deviation as indicated in the figure legend. Pre- and postoperative values were compared by Wilcoxon test, and analysis of differences between trauma patients and healthy donors were evaluated by Mann Whitney U-test. For multiple group analysis the Wilcoxon test was applied which is independent of normality distribution of the data. All tests were calculated two-sided. Data analysis and statistics were performed using the Statistical Package for Social Sciences (SPSS) version 11.0 for Windows (SPSS Headquarters, Chicago, Ill., USA). The statistical procedure is indicated in the figure legend. A P-value <0.05 was considered as statistically significant.
Results
Severely injured patients primarily admitted to the local trauma department and the surgical intensive care unit were monitored regarding the immunologic status by measuring HLA-DR expression on monocytes by means of flow cytometry and the ex vivo TNFα synthesis of endotoxin-stimulated blood. Sixteen of these fulfilled the inclusion criteria with a mean ISS of 39±9 points and mean age of 46±17 years. Erythrocyte concentrates (2,220±852 ml) and fresh frozen plasma (4,018±2750 ml) were transfused within the first 48 h in these patients. Ninety-five point one percent developed sepsis and 52.9% a multiple organ failure (MOF) as defined in the method section. Two patients died due to persisting MOF, and a third died because of cardiac failure after secondary surgery. The patients’ data are summarised in Table 1.
Whereas 62.5% of the patients required primary surgery during the first 6 h after trauma, 37.5% could be admitted to the surgical intensive care unit directly after the emergency room treatment and completion of the diagnostic work-up. Patients with or without primary surgery did not differ significantly in ISS (42±10 with primary surgery vs 35±7 without primary surgery). Secondary surgery consisted of unreamed intramedullary nailing of long bone fractures (n=5), osteosynthesis of the pelvic girdle (n=4), internal spine stabilisation (n=2), osteosynthesis of peripheral fractures (n=6), plastic reconstructive surgery (n=3),and septic focus clearance (n=5).
Healthy donors had a mean age of 36.6±13.8 (mean ± SD) years and included six males and six females. When compared to healthy donors the patients revealed significantly diminished HLA-DR expression on monocytes and ex vivo TNFα synthesis (Fig. 1). The HLA-DR expression on monocytes on the day after admittance to the intensive care unit was depressed to the same degree in patients with and those without surgery at the day of initial trauma (441±62 MFI HLA-DR with primary surgery vs 429±40 MFI HLA-DR without primary surgery). The TNFα-producing capacity of whole blood was lower in patients’ samples after primary surgery (234±285 with primary surgery vs 101±88 ng/ml TNFα without primary surgery ), although this difference did not reach level of significance.
A HLA-DR expression on monocytes and B ex vivo TNFα synthesison day 1 after trauma and before surgery and HLA-DR expression on monocytes and ex vivo TNFα synthesis after secondary surgery. Whole blood cultures drawn from severely injured patients on the 1st day after trauma (day 1; n=16), 1–2 days before secondary surgery (pre-; 24 events in 16 patients), 1–2 days after secondary surgery (post-; 24 events in 16 patients), 3–4 days after secondary surgery (21 events in 16 patients), and from healthy donors (n=12) were in vitro stimulated with 10 ng/ml LPS for 20 h. LPS-induced TNFα synthesis is expressed in pg/ml in the supernatant (boxplots with median, 75th and 90th percentile). Dots represent values out of 90th percentile, extreme values are shown as numbers. In the same blood samples HLA-DR expression on monocytes was analysed by flow cytometry and is expressed as MFI (median, 75th and 90th percentile ). ** indicates statistical difference to healthy volunteers with a P-value<0.01 in a Mann Whitney U-test. ## indicates statistical difference to preoperative values with a P-value <0.01 (Wilcoxon test). && shows statistical difference between day 1 and preoperative samples with a P-value <0.01(Wilcoxon test)
Definitive surgical treatment was generally performed after the second week after trauma, on average 17.5±10.9 days after trauma. Shortly before surgery the ex vivo TNFα synthesis was significantly higher than on day 1 after trauma and no longer significantly different from that of healthy donors. HLA-DR expression on monocyte before surgery was still lower than that of healthy donors, but significantly higher than on day 1 after injury (Fig. 1).
When performed in the second week after trauma surgical interventions (including all operations) did not cause a significant change in HLA-DR expression on monocytes or ex vivo LPS-induced TNFα synthesis (Fig. 1). Three to five days after secondary surgery the HLA-DR expression on monocytes significantly increased in comparison to preoperative values, indicating a normalisation of the immune function (Fig. 1A).
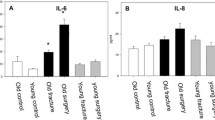
A more detailed analysis of the influence of secondary surgery on the immune system after trauma was performed by taking the character of the operation into account. Three categories of surgical intervention defined as described in the method section demonstrated different immunological response patterns. Surgical intervention performed to clear septic foci consisted of drainage of perineal abscess (2×), infected hematoma after acetabulum osteosynthesis, purulent sinusitis, and intraabdominal abscess after splenectomy. Focus clearance generally improved immune functions reflected by an increase in HLA-DR expression on monocytes within 1–3 days after surgery. Ex vivo TNFα synthesis of whole blood after LPS stimulation was also slightly increased after focus clearance (Fig. 2). Minor surgery had no influence on the immune system in the second week after trauma: HLA-DR expression on monocytes as well as ex vivo LPS-stimulated TNFα production even tended to rise towards normal levels despite of the surgical intervention (Fig. 3). In contrast, more traumatising major surgery significantly reduced HLA-DR expression on monocytes. Ex vivo TNFα synthesis 1–2 days after the operation was not significantly decreased (Fig. 4). However, these disturbances of the immune response were reversible, since both ex vivo TNFα-producing capacity and HLA-DR expression on monocytes reached preoperative levels within 3–5 days after surgery (Fig. 4).
HLA-DR expression on monocytes and ex vivo TNFα synthesis after septic focus clearance. Heparinised blood cultures were drawn from severely injured patients on the day before surgical septic focus clearance (five events in four patients) and 1–2 days after surgery. Data are expressed as median, 75th and 90th percentile. For details see Fig. 1. No statistical evaluation was performed because of small sample numbers
HLA-DR expression on monocytes and ex vivo TNFα synthesis after minor secondary surgery. Heparinised blood cultures were drawn from severely injured patients on the day before minor secondary surgery (nine events in eight patients) and 1–2 days after surgery. Data are expressed as median, 75th and 90th percentile. For details see Fig. 1. No statistical difference to preoperative values was found (Wilcoxon test)
HLA-DR expression on monocytes and ex vivo TNFα synthesis after major secondary surgery. Heparinised blood cultures were drawn from severely injured patients on the day before major secondary surgery (ten events in nine patients) and 1–2 days and 3–4 days (eight events in seven patients) after surgery. Data are expressed as median, 75th and 90th percentile. For details see Fig. 1. # indicates statistical difference to preoperative values with a P-value <0.05 (Wilcoxon test). Statistical difference between blood sample drawn 3–4 days after surgery and other time points were not found
Serum IL-10 levels were found to be elevated initially after injury as well as at the time point of secondary surgery (Table 2). However, secondary surgery itself lowered serum IL-10 levels in parallel to a reduction in HLA-DR expression and TNFα-producing capacity (Table 2). The lowest IL-10 serum levels were found in patients after clearance of septic foci.
Discussion
The present study shows that major secondary surgery after severe trauma disturbs the immune response of these patients. HLA-DR expression on monocytes and the ex vivo TNFα synthesis of LPS-stimulated whole blood were used as marker for the status of the immune response. Both markers have been extensively studied in severely injured patients. The degree of depression of HLA-DR expression of monocytes and the ex vivo TNFα synthesis has been reported to correlate with the degree of injury [18, 19]. In patients with sepsis the same markers have a high negative prognostic value [20]. Low HLA-DR expression after major elective resectional surgery have been shown to be associated with the development of sepsis after surgery [21] underlining the importance of this marker of the immune function.
In this study, secondary surgery in severely injured patients was generally performed not before the second week after trauma. Primary surgery was only performed in a minimally traumatising manner as a damage control procedure. Since there was no difference in HLA-DR expression after admittance on the ICU between the patients with and those without primary surgery, one could speculate that the surgical stress of a damage control surgery in the initial phase after trauma does not further decrease immune functions. The TNFα-producing capacity tends to be lower, although not significantly, in patients with primary damage control surgery. Generally, there exists a growing body of evidence that underlines the impact of additional surgical stress in the initial treatment of severely inured patients. A large retrospective study with more than 4,000 severely injured patients revealed a higher incidence of posttraumatic multiple organ failure (MOF) in patients with secondary surgery on day 2–4 compared to patients with definitive surgical treatment on day 6–8 after trauma [14]. Other studies demonstrated a high predictive value of elevated CRP serum levels for multiple organ failure after secondary surgery in severely injured patients [22]. In our study we observed a still suppressed HLA-DR expression and ex vivo TNFα producing capacity at the time point of surgery even with a delayed treatment regime. A downmodulation of HLA-DR expression on monocytes for a period of 2 weeks after injury is in line with other studies of this marker in trauma patients [23]. At the time point of definitive surgical treatment minor surgery did not influence the analysed immune functions, whereas more traumatising surgery as intramedullary nailing still caused a depression of HLA-DR expression on monocytes and a reduction of the ex vivo LPS-induced TNFα synthesis. Corresponding surgery-induced changes of markers of the inflammatory response such as circulating IL-6, interleukin-8 (IL-8) and elastase have already been reported in trauma patients [24]. In this study with severely injured patients, operations on the pelvic girdle and femur caused higher levels of circulating IL-6, IL-8, and elastase compared to maxillofacial surgery, for example. Obviously, more traumatizing secondary surgery trauma in severely injured patients causes both a systemic inflammatory response marked by elevated systemic levels of, for example, IL-6 and a parallel anti-inflammation as HLA-DR expression or cytokine-producing capacity.
Suppression of cytokine-producing capacity after accidental and surgical trauma has been found to be associated with the appearance of a cytokine-inhibitory activity in the serum of these patients [4]. While some studies suggested the involvement of the anti-inflammatory activity mediators IL-10 or transforming growth factor (TGF) ß as the dominant cytokine-suppressive mechanism [25, 26], other studies could exclude IL-10 and TGFß as the only reason for the diminished cytokine-producing capacity after injury or surgery [27, 28]. Decrease HLA-DR surface expression on monocytes by serum from patients with sepsis has also been contributed to the action of IL-10 [7]. In the present study the decreased ex vivo TNFα-producing capacity and HLA-DR expression on monocytes after major secondary surgery was not accompanied by an increase in serum IL-10, which supports the involvement of additional mechanisms.
It remains to be elucidated whether this depression of immune functions represents a necessary counter regulatory mechanism or renders the patients more susceptible to infectious complications. Studies with immune modulating substances such as interferon γ, interleukin-12 (IL-12), granulocyte colony-stimulating factor (G-CSF) or granulocyte-macrophage colony-stimulating factor (GM-CSF) could answer these questions. Preoperative immune modulation with G-CSF in patients undergoing esophagectomy could reduce the rate of infections [29, 30]. A study with low-dose GM-CSF given perioperatively in patients operated on for primary colorectal carcinoma showed that this factor could counteract surgery-induced depression of HLA-DR expression on monocytes [11]. However, further studies with immune modulating substances and detailed analysis of immune functions need to be performed.
Surgery for the clearance of septic foci seems to improve immune functions rapidly. The reduction of the bacterial burden does not only support the immune system to definitively eliminate the remaining infectious agents, but also improves the immune response itself directly, which underlines the importance of a basic surgical principle from an immunologic point of view.
Summarising, we found that delayed secondary minor surgery in severely injured patients caused no change in immune functions, while major surgery suppresses the immune functions even if performed in stable patients 2 weeks after trauma. Septic focus clearance, as expected, improves the immune response in terms of HLA-DR expression and ex vivo TNFα synthesis.
References
Ditschkowski M, Kreuzfelder E, Rebmann V, Ferencik S, Majetschak M, Schmid EN, Obertacke U, Hirche H, Schade UF, Grosse-Wilde H (1999) HLA-DR expression and soluble HLA-DR levels in septic patients after trauma. Ann Surg 229:246–254
Ditschkowski M, Kreuzfelder E, Majetschak M, Obertacke U, Schade FU, Grosse-Wilde H (1999) Reduced B cell HLA-DR expression and natural killer cell counts in patients prone to sepsis after injury. Eur J Surg 165:1129–1133
Faist E, Schinkel C, Zimmer S (1996) Update on the mechanisms of immune suppression of injury and immune modulation. World J Surg 20:454–459
Majetschak M, Flach R, Heukamp T, Jennissen V, Obertacke U, Neudeck F, Schmit-Neuerburg KP, Schade FU (1997) Regulation of whole blood Tumor Necrosis Factor production upon endotoxin stimulation after severe blunt trauma. J Trauma 43:1-8
Keel M, Schregenberger N, Steckholzer U, Ungethum U, Kenney J, Trentz O, Ertel W (1996) Endotoxin tolerance after severe injury and its regulatory mechanisms. J Trauma 41:430–437
Giannoudis PV, Smith RM, Perry SL, Windsor AJ, Dickson RA, Bellamy MC (2000) Immediate IL-10 expression following major orthopaedic trauma: relationship to anti-inflammatory response and subsequent developement of sepsis. Int Care Med 26:1076–1081
Fumeaux T, Pugin J (2002) Role of Interleukin-10 in the Intracellular sequestration of human leukocyte antigen-DR in monocytes during septic shock. Am J Respir Crit Care Med 166:1475–1482
Asadullah K, Woiciechowsky C, Doecke WD, Liebenthal C, Wauer H, Kox W, Volk HD, Vogel S, Von Baehr R (1995) Immunodepression following neurosurgical procedures. Crit Care Med 23:1976–1983
Hiesmayr MJ, Spittler A, Lassnigg A, Berger R, Laufer G, Kocher A, Artemiou O, Boltz-Nitulescu G, Roth E (1999) Alterations in the number of circulating leucocytes, phenotype of monocytes and cytokine production in patients undergoing cardiothoracic surgery Clin Exp Immunol 115:315–323
Decker D, Schondorf M, Bidlingmaier F, Hirner A, von Ruecker AA (1996) Surgical stress induces a shift in the type-1/type-2 T-helper cell balance, suggesting down-regulation of cell-mediated and up-regulation of antibody-mediated immunity commensurate to the trauma. Surgery 119:316–325
Mels AK, Statius Muller MG, van Leeuwen PA, van Blomberg BM, Scheper RJ, Cuesta MA, Beelen RH, Meijer S (2001) Immune-stimulating effects of low-dose perioperative recombinant granulocyte-macrophage colony-stimulating factor in patients operated on for primary colorectal carcinoma. Br J Surg 88:539–544
Berger D, Bolke E, Seidelmann M, Beger HG (1997) Time-scale of interleukin-6, myeloid related proteins (MRP), C reactive protein (CRP), and endotoxin plasma levels during the postoperative acute phase reaction. Shock 7:422–426
Pape HC, Schmidt RE, Rice J, van Griensven M, das Grupta R, Krettek C, Tscherne H (2000) Biochemical changes after trauma and skeletal surgery of the lower extremity: quantification of the operative burden. Crit Care Med 28:3441–3448
Pape HC, Stalp M, van Griensven M, Weinberg A, Dahlweit N, Tscherne H (1999) Optimal timing for secondary surgery in polytrauma patients: an evaluation of 4314 serious-injury cases. Chirurg 70:1287–1293
Trupka A, Waydhas C, Nast-Kolb D, Schweiberer L (1994) Early intubation in severely injured patients. Eur J Emerg Med 1:1-8
Bone, RC, Balk, RA, Cerra, FB, Dellinger RP, Fein AM, Knaus WA, Schein RM, Sibbald WJ (1992). Definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. The ACCP/SCCM Consensus Conference Committee. American College of Chest Physicians/Society of Critical Care Medicine. Chest 101:1644–1655
Vincent JL, Moreno R, Takala J, Willatts S, De Mendonca A, Bruining H, Reinhart CK, Suter PM, Thijs LG (1996). The SOFA (Sepsis-related Organ Failure Assessment) Score to describe organ dysfunction/failure. On behalf of the Working Group on Sepsis-Related Problems of the European Society of Intensive Care Medicine. Intensive Care Med 22:707–710
Hershman MJ, Cheadle WG, Wellhausen SR, Davidson PF, Polk HC, Jr (1990) Monocyte HLA-DR antigen expression characterises clinical outcome in the trauma patient. Br. J. Surg. 77:204–207
Majetschak M, Flach R, Kreuzfelder E, Jennissen V, Obertacke U, Neudeck F, Schmit-Neuerburg KP, Schade FU (1999) The extent of traumatic damage determines a graded depression of the endotoxin responsiveness of peripheral blood mononuclear cells from patients with blunt injuries. Crit Care Med 27:313–318
Volk HD, Thieme M, Heym S, Doecke WD, Ruppe U, Tausch W, Manger D, Zuckermann S, Golosubow A, Nieter B (1991) Alterations in function and phenotype of monocytes from patients with septic disease—predictive value and new therapeutic strategies. Behring Inst Mitt 88:208–215
Wakefield CH, Carey PD, Foulds S, Monson JR, Guillou PJ (1993) Changes in major histocompatibility complex class II expression in monocytes and T cells of patients developing infection after surgery. Br J Surg 80:205–209
Waydhas C, Nast-Kolb D, Trupka A, Zettl R, Kick M, Wiesholler J, Schweiberer L, Jochum M (1996) Posttraumatic inflammatory response, secondary operations, and late multiple organ failure. J Trauma 40:624–630
Boelens PG, Houdijk AP, Fonk JC, Nijveldt RJ, Ferwerda CC, Von Blomberg-Van der Flier BM, Thijs LG, Haarman HJ, Puyana JC, Van Leeuwen PA (2002) Glutamine-Enriched Enteral Nutrition Increases HLA-DR Expression on Monocytes of Trauma Patients. J Nutr 132:2580–2586
Waydhas C, Nast Kolb D, Kick M, Trupka A, Zettl R, Wiesholler H, Schmidbauer S, Jochum M, Schweiberer L (1995) Postoperative homeostatic imbalance after trauma surgical interventions of various degrees in polytrauma. Unfallchirurg 98:455–463
Miller-Graziano CL, Szabo G, Griffey K, Metha B, Kodys K, Catalano D (1991) Role of elevated monocyte transforming growth factor beta (TGFß) production in posttrauma immunosuppression. J Clin Immunol 11:95–102
Ogata M, Okamoto K, Kohriyama K, Kawasaki T, Itoh H, Shigematsu A (2000) Role of Interleukin-10 on hyporesponsiveness of endotoxin during surgery. Crit Care Med 28:3166–3170
Majetschak M, Boergermann J, Waydhas C, Obertacke U, Nast-Kolb D, Schade FU (2000) Whole blood TNFα production and its relationship to systemic concentrations of IL-4, IL-10 and TGF-ß1 in multiply in blunt trauma victims. Crit Care Med 28:1847–1853
Boergermann J, Friedrich I, Flohé S, Spillner J, Majetschak M, Kuss O, Sablotzki A, Feldt T, Reidemeister JC, Schade FU (2002) Tumor necrosis factor-α production in whole blood after cardiopulmonary bypass: downregulation caused by circulating cytokine-inhibitory activities. J Thorac Cardiovasc Surg 124:608–617
Hubel K, Mansmann G, Schafer H, Oberhauser F, Diehl V, Engert A (2000) Increase of anti-inflammatory cytokines in patients with esophageal cancer after perioperative treatment with G-CSF. Cytokine 12:1797–1800
Schafer H, Hubel K, Bohlen H, Mansmann G, Hegener K, Richarz B, Oberhauser F, Wassmer G, Holscher AH, Pichlmaier H, Diehl V, Engert A (2000) Perioperative treatment with filgrastim stimulates granulocyte function and reduces infectious complications after esophagectomy. Ann Hematol 79:143–151
Acknowledgement
The IFORES program of the university of Essen financially supported this work.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Flohé, S., Lendemans, S., Schade, FU. et al. Influence of surgical intervention in the immune response of severely injured patients. Intensive Care Med 30, 96–102 (2004). https://doi.org/10.1007/s00134-003-2041-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-003-2041-3