Abstract
Purpose
Our goal is to assess the prevalence of questioning about the appropriateness of initiating or maintaining life-sustaining treatments (LST) in French-speaking paediatric intensive care units (PICUs) and to evaluate time utilisation related to decision-making processes (DMP).
Methods
18-month, multicentre, prospective, descriptive, observational study in 15 French-speaking PICUs.
Results
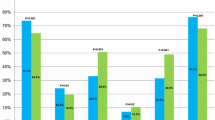
Among the 5,602 children admitted, 410 died (7.3%), including 175 after forgoing LST (42.7% of deaths). LST was questioned in 308 children (5.5%) with a prevalence of 13.3 per 100 patient-days. More than 30% of children survived despite the appropriateness of LST being questioned (23% despite a decision to forgo treatment). Median caregiver time spent on making and presenting the decisions was 11 h per child.
Conclusions
In this study, on any given day in each 10-bed PICU, there was more than one child for whom a DMP was underway. Of children, 23% survived despite a decision to forgo LST being made, which underlines the need to elaborate a care plan for these children. Also, DMP represented a large amount of staff time that is undervalued but necessary to ensure optimal palliative practice in PICU.

Similar content being viewed by others
Abbreviations
- DMP:
-
Decision-making process
- DRNO:
-
Do-not-resuscitate order
- GFRUP:
-
Groupe Francophone de Réanimation et Urgence Pédiatriques (French-Speaking Group of Paediatric Intensive and Emergency Care)
- NPICU:
-
Neonatal and paediatric intensive care unit
- PICU:
-
Paediatric intensive care unit
- PIM2 score:
-
Paediatric Index of Mortality score
- POPC score:
-
Paediatric Overall Performance Category score
References
McCallum DE, Byrne P, Bruera E (2000) How children die in hospital. J Pain Symptom Manage 20:417–423
van der Wal ME, Renfurm LN, van Vught AJ, Gemke RJ (1999) Circumstances of dying in hospitalized children. Eur J Pediatr 158:560–565
Kipper DJ, Piva JP, Garcia PC, Einloft PR, Bruno F, Lago P, Rocha T, Schein AE, Fontela PS, Gava DH, Guerra L, Chemello K, Bittencourt R, Sudbrack S, Mulinari EF, Morais JF (2005) Evolution of the medical practices and modes of death on pediatric intensive care units in southern Brazil. Pediatr Crit Care Med 6:258–263
Althabe M, Cardigni G, Vassallo JC, Allende D, Berrueta M, Codermatz M, Cordoba J, Castellano S, Jabornisky R, Marrone Y, Orsi MC, Rodriguez G, Varon J, Schnitzler E, Tamusch H, Torres JM, Vega L (2003) Dying in the intensive care unit: collaborative multicenter study about forgoing life-sustaining treatment in Argentine pediatric intensive care units. Pediatr Crit Care Med 4:164–169
Lago PM, Piva JP, Kipper DJ, Garcia PC, Pretto C, Giongo M, Branco R, Bueno F, Traiber C, Araujo T, Wortmann D, Librelato G, Soardi D (2005) Life support limitation at three pediatric intensive care units in southern Brazil. J Pediatr (Rio J) 81:11–17
Vernon DD, Dean M, Timmons OD, Banner W, Allen-Webb EM (1993) Modes of death in the pediatric intensive care unit: withdrawal and limitation of supportive care. Crit Care Med 21:1798–1802
Burns JP, Mitchell C, Outwater KM, Geller M, Griffith JL, Todres ID, Truog RD (2000) End-of-life care in the pediatric intensive care unit after the forgoing of life-sustaining treatment. Crit Care Med 28:3060–3066
Garros D, Rosychuk RJ, Cox PN (2003) Circumstances surrounding end of life in a pediatric intensive care unit. Pediatrics 112:e371–e379
Adams AS, Soumerai SB, Lomas J, Ross-Degnan D (1999) Evidence of self-report bias in assessing adherence to guidelines. Int J Qual Health Care 11:187–192
Sprung CL, Cohen SL, Sjokvist P, Baras M, Bulow HH, Hovilehto S, Ledoux D, Lippert A, Maia P, Phelan D, Schobersberger W, Wennberg E, Woodcock T (2003) End-of-life practices in European intensive care units: the ethicus study. JAMA 290:790–797
Devictor DJ, Nguyen DT (2004) Forgoing life-sustaining treatments in children: a comparison between Northern and Southern European pediatric intensive care units. Pediatr Crit Care Med 5:211–215
Sprung CL, Woodcock T, Sjokvist P, Ricou B, Bulow HH, Lippert A, Maia P, Cohen S, Baras M, Hovilehto S, Ledoux D, Phelan D, Wennberg E, Schobersberger W (2008) Reasons, considerations, difficulties and documentation of end-of-life decisions in European intensive care units: the ETHICUS Study. Intensive Care Med 34:271–277
Burns JP, Mitchell C, Griffith JL, Truog RD (2001) End-of-life care in the pediatric intensive care unit: attitudes and practices of pediatric critical care physicians and nurses. Crit Care Med 29:658–664
Zawistowski CA, DeVita MA (2004) A descriptive study of children dying in the pediatric intensive care unit after withdrawal of life-sustaining treatment. Pediatr Crit Care Med 5:216–223
American Academy of Pediatrics (2000) American Academy of Pediatrics. Committee on Child Abuse and Neglect and Committee on Bioethics. Foregoing life-sustaining medical treatment in abused children. Pediatrics 106:1151–1153
Truog RD, Cist AF, Brackett SE, Burns JP, Curley MA, Danis M, DeVita MA, Rosenbaum SH, Rothenberg DM, Sprung CL, Webb SA, Wlody GS, Hurford WE (2001) Recommendations for end-of-life care in the intensive care unit: The Ethics Committee of the Society of Critical Care Medicine. Crit Care Med 29:2332–2348
Royal College of Paediatrics and Child Health (2004) Withholding or Withdrawing Life Sustaining Treatment in Children: A Framework for Practice (second edition). Available online at http://wwwrcpchacuk/docaspx?id_Resource=2002
Hubert P, Canoui P, Cremer R, Leclerc F (2005) Limitations et arrêts des traitements actifs en réanimation pédiatrique: recommandations du GFRUP. Arch Pediatr 12:1501–1508
Truog RD, Campbell ML, Curtis JR, Haas CE, Luce JM, Rubenfeld GD, Rushton CH, Kaufman DC (2008) Recommendations for end-of-life care in the intensive care unit: a consensus statement by the American College [corrected] of Critical Care Medicine. Crit Care Med 36:953–963
Shemie SD, Pollack MM, Morioka M, Bonner S (2007) Diagnosis of brain death in children. Lancet Neurol 6:87–92
Slater A, Shann F, Pearson G (2003) PIM2: a revised version of the Paediatric Index of Mortality. Intensive Care Med 29:278–285
Leteurtre S, Martinot A, Duhamel A, Proulx F, Grandbastien B, Cotting J, Gottesman R, Joffe A, Pfenninger J, Hubert P, Lacroix J, Leclerc F (2003) Validation of the paediatric logistic organ dysfunction (PELOD) score: prospective, observational, multicentre study. Lancet 362:192–197
Fiser DH (1992) Assessing the outcome of pediatric intensive care. J Pediatr 121:68–74
Martinot A, Grandbastien B, Leteurtre S, Duhamel A, Leclerc F (1998) No resuscitation orders and withdrawal of therapy in French paediatric intensive care units. Groupe Francophone de Réanimation et d’Urgences Pédiatriques. Acta Paediatr 87:769–773
Devictor DJ, Nguyen DT (2001) Forgoing life-sustaining treatments: how the decision is made in French pediatric intensive care units. Crit Care Med 29:1356–1359
British Medical Association (1999) Withholding and withdrawing life-prolonging medical treatment: guidance for decision making. BMJ Books, London
Ethics Committee of the Society of Critical Care Medicine (1997) Consensus statement of the Society of Critical Care Medicine’s Ethics Committee regarding futile and other inadvisable treatments. Crit Care Med 25:887–891
GFRUP (2002) Limitations et arrêts des traitements en réanimation pédiatrique. Repères pour la pratique. In: Fondation de France (ed) Book Limitations et arrêts des traitements en réanimation pédiatrique. Repères pour la pratique. Paris
Fassier T, Darmon M, Laplace V, Chevret S, Schlemmer B, Pochard F, Azoulay E (2007) One-day quantitative cross-sectional study of family information time in 90 intensive care units in France. Crit Care Med 35:177–183
(2005) Loi n° 2005-370 du 22 avril 2005 relative aux droits des malades et à la fin de vie. Journal Officiel de la République Française du 23 avril 2005 N°95:7089
Sykes N, Thorns A (2003) The use of opioids and sedatives at the end of life. Lancet Oncol 4:312–318
Ferrand E, Robert R, Ingrand P, Lemaire F (2001) Withholding and withdrawal of life support in intensive-care units in France: a prospective survey. French LATAREA Group. Lancet 357:9–14
Cremer R, Fourestié B, Binoche A, Botte A, Moutel G, Leclerc F (2008) Que deviennent les décisions de limitation ou d’arrêt des traitements actifs quand les enfants sortent vivants de réanimation pédiatrique? Arch Pediatr 17:1174–1182
Cremer R, Binoche A, Moutel G, Fourestie B, Botte A, Le Grand-Sébille C, Leclerc F (2009) Pourquoi les décisions de limitation des traitements en réanimation ne sont elles pas partagées avec les professionnels assurant les soins de l’enfant avant et après la réanimation. Arch Pediatr 16:1233–1244
Fraser LK, Fleming T, Miller M, Draper ES, McKinney PA, Parslow RC (2010) Palliative care discharge from paediatric intensive care units in Great Britain. Palliat Med 24:608–615
Carnevale FA, Canoui P, Hubert P, Farrell C, Leclerc F, Doussau A, Seguin MJ, Lacroix J (2006) The moral experience of parents regarding life-support decisions for their critically-ill children: a preliminary study in France. J Child Health Care 10:69–82
(2006) Décret n°2006-120 du 6 février 2006 relatif à la procédure collégiale prévue par la loi n° 2005-370 du 22 avril 2005 relative aux droits des malades et à la fin de vie et modifiant le code de la santé publique (dispositions réglementaires) Journal Officiel de la République Française du 7 février 2006 N°32:1974
Acknowledgments
This work was supported by grants from the Réseau Mère-Enfant de la Francophonie and the French Ministry of Health (PHRC AOM08179–NI07014). We thank the investigators for their record keeping and Dr. Susanne Rogers for correcting the manuscript.
Conflict of interest
The authors declare that they have no competing interests.
Author information
Authors and Affiliations
Consortia
Corresponding author
Appendix: GFRUP’s study group on forgoing treatments
Appendix: GFRUP’s study group on forgoing treatments
Data were collected in the NPICU/PICUs of the following centres: American Memorial Hospital, CHU de Reims, France; Hôpital Charles Nicolle, CHU de Rouen, France; Hôpital Arnaud de Villeneuve, CHU de Montpellier, France; Hôpital Clocheville, CHU de Tours, France; Hôpital des enfants, CHU de Toulouse, France; Hôpital Hautepierre, CHU de Strasbourg, France; Hôpital Jeanne de Flandre, CHU de Lille, France; Hôpital Femme Mère-enfant, Hospices Civils de Lyon, France, France; Hôpital Morvan, CHU de Brest, France; Hôpital Necker, Assistance Publique-Hôpitaux de Paris, France; Hôpital Nord, CHU de Grenoble, France; Hôpital Reine Fabiola, Bruxelles, Belgium; Hôpital Robert Debré, Assistance Publique-Hôpitaux de Paris, France; Hôpital Saint Pierre, CHU de Besançon, France; Hôpital Trousseau, Assistance Publique-Hôpitaux de Paris, France.
Investigators were: D. Biarent (Bruxelles, Belgium), T. Blanc (Rouen, France), S. Cantagrel (Tours, France), R. Cremer (Lille, France); S. Dauger (Paris, France), P. Desprez (Strasbourg, France), M. Dobrzynski (Brest, France), G. Emériaud (Grenoble, France), P. Hubert (Paris, France), C. Milesi (Montpellier, France), S. Renolleau (Paris, France), N. Richard (Lyon, France), M. Roque-Gineste (Toulouse, France), O. Noizet-Yverneau (Reims, France), D. Stamm (Lyon, France), I. Wroblewski (Besançon, France).
Rights and permissions
About this article
Cite this article
Cremer, R., Hubert, P., Grandbastien, B. et al. Prevalence of questioning regarding life-sustaining treatment and time utilisation by forgoing treatment in francophone PICUs. Intensive Care Med 37, 1648–1655 (2011). https://doi.org/10.1007/s00134-011-2320-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-011-2320-3