Abstract
Purpose
Catheter-directed thrombolysis (CDT) is a highly effective approach in the treatment of deep venous thrombosis (DVT). There are no data on the primary use of CDT with argatroban and tissue plasminogen activator (tPA) in patients without heparin-induced thrombocytopenia (HIT). The aim of this study was to evaluate the efficacy and safety of the combined administration of argatroban and tPA during CDT for massive DVT in patients without HIT.
Methods
Thirty-three patients with massive symptomatic iliac and femoropopliteal DVT underwent CDT with tPA and argatroban within 28 ± 6 h of presentation. The dose of tPA was 0.75–1 mg/h through the infusion port and that of argatroban at 0.3–1 μg/kg/min through the side port of the sheath. The patients were evaluated for the efficacy and safety of CDT and recurrent symptomatic venous thromboembolism (VTE) at a mean follow-up of 22 months.
Results
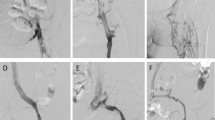
There was no bleeding or iatrogenic pulmonary embolism with the CDT regimen we used. Grade III lysis (complete resolution of thrombus on venography) was achieved in 30 patients (91 %). In 3 patients with additional inferior vena cava filter thrombosis, further thrombectomy of the filter was required. No patient developed recurrent VTE.
Conclusion
Concomitant administration of argatroban and tPA is a highly safe and effective regimen for CDT for massive DVT.

Similar content being viewed by others
References
Pollack C (2011) Advanced management of acute ileofemoral deep venous thrombosis: emergency department and beyond. Ann Emerg Med 57:590–599
Sharifi M, Bay C, Mehdipour M, Sharifi J, TORPEDO Investigators (2012) Thrombus obliteration by rapid percutaneous endovenous intervention in deep venous occlusion (TORPEDO) trial: midterm results. J Endovasc Ther 19:273–280
Wong CK, White HD (2007) Direct antithrombins: mechanisms, trials, and role in contemporary interventional medicine. Am J Cardiovasc Drugs 7:249–257
Jang I, Brown D, Giugliani R et al (1999) A multicenter, randomized study of argatroban versus heparin as adjunct to tissue plasminogen activator (TPA) in acute myocardial infarction: myocardial infarction with novastan and TPA (MINT) study. Am Coll Cardiol 33:1879–1885
Valji K, Arun K, Bookstein JJ (1995) Use of a direct thrombin inhibitor (argatroban) during pulse-spray thrombolysis in experimental thrombosis. J Vasc Interv Radiol 6:91–95
Sharifi M, Spagnolo K, Lawson D et al (2012) Low dose argatroban and tPA in the treatment of massive iliac and femoropopliteal deep vein thrombosis. Catheteriz Cardiovasc Interv 79:S 29
Patterson BO, Hinchliffe R, Loftus IM et al (2010) Indications for catheter-directed thrombolysis in the management of acute proximal deep venous thrombosis. Arterioscler Thromb Vasc Biol 30:669–674
Maldonado A (2009) Argatroban and catheter-directed thrombolysis with alteplase for limb- and graft-threatening thromboses in a patient with a history of HIT. Am J Hematol 84:251–253
Turba UC, Bozlar U, Simsek S (2007) Catheter-directed thrombolysis of acute lower extremity arterial thrombosis in a patient with heparin-induced thrombocytopenia. Catheter Cardiovasc Interv 70:1046–1050
Boeve TJ, Reed GL, de Oliveira NC et al (1998) Comparison of argatroban and hirudin for the reperfusion of thrombotic arterial occlusion by tissue plasminogen activator. J Thromb Thrombolysis 6:103–108
Barreto AD, Alexandrov AV, Lyden PD et al (2011) The argatroban and tPA stroke study: final results of a pilot safety study. Stroke 42:770–775
Mewissen MW, Seabrook GR, Meissner MH et al (1999) Catheter-directed thrombolysis for lower extremity deep venous thrombosis: report of a national multicenter registry. Radiology 211:39–49
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sharifi, M., Bay, C., Nowroozi, S. et al. Catheter-directed Thrombolysis with Argatroban and tPA for Massive Iliac and Femoropopliteal Vein Thrombosis. Cardiovasc Intervent Radiol 36, 1586–1590 (2013). https://doi.org/10.1007/s00270-013-0569-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-013-0569-3