Abstract
Background
Breast-conserving surgery (BCS) requires clear surgical margins to minimize local recurrence. We sought to identify groups of patients at higher risk of involved margins who might benefit from preoperative counselling and/or more generous excision at the first operation.
Methods
We reviewed demographic, clinical, radiological and pathological records of all women diagnosed with ductal carcinoma in situ (DCIS) or invasive cancer (IC) through a population-based breast screening program in Melbourne, Australia between 1994 and 2005.
Results
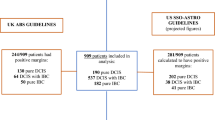
A total of 2,160 women were diagnosed with DCIS or IC. We excluded 199 who had mastectomy (TM) as initial procedure or had missing data. Three hundred and thirteen had a diagnostic biopsy. Of 1,648 women who had BCS after a preoperative diagnosis of DCIS or IC, 13.5% had involved margins, 16.6% had close (≤1 mm), and 69.8% clear (>1 mm) margins. Of the patients, 281/1,648 (17.1%) underwent re-excision, of whom 93 (33.1%) had residual disease identified. Mammographic microcalcifications (P < 0.0001), absence of a mammographic mass (P = 0.002), presence of DCIS (P < 0.0001), high tumour grade (P < 0.0001), large size (P < 0.0001), multifocal disease (P < 0.0001) and lobular histology (P = 0.005) were associated with involved margins. Microcalcifications (odds ratio [OR] 1.97), large size (OR 4.22) and multifocal disease (OR 2.85) were independently associated with involved margins. Residual disease was associated with involved margins (P < 0.0001), presence of DCIS (P = 0.05) and large tumour size (P = 0.01).
Conclusion
After BCS, patients with mammographic microcalcifications, larger tumour size and multifocal tumours are more likely to have involved margins. Patients with involved margins, large tumour size and/or a DCIS component are more likely to have residual disease on re-excision.
Similar content being viewed by others
References
van Dongen JA, Voogd AC, Fentiman IS, et al. Long-term results of a randomized trial comparing breast-conserving therapy with mastectomy: European Organization for Research and Treatment of Cancer 10801 trial. J Natl Cancer Inst 2000; 92:1143–50.
Fisher B, Anderson S, Bryant J, et al. Twenty-year follow-up of a randomized trial comparing total mastectomy, lumpectomy, and lumpectomy plus irradiation for the treatment of invasive breast cancer. New Engl J Med 2002; 347:1233–41.
Clarke M, Collins R, Darby S, et al. Effects of radiotherapy and of differences in the extent of surgery for early breast cancer on local recurrence and 15-year survival: an overview of the randomised trials. Lancet 2005; 366:2087–106.
Cady B, Stone MD, Schuler JG, et al. The new era in breast cancer. Invasion, size, and nodal involvement dramatically decreasing as a result of mammographic screening. Arch Surg 1996; 131:301–8.
Veronesi U, Banfi A, Salvadori B, et al. Breast conservation is the treatment of choice in small breast cancer: long-term results of a randomized trial. Eur J Cancer 1990; 26:668–70.
Samnakay N, Tinning J, Ives A, et al. Rates for mastectomy are lower in women attending a breast-screening programme. ANZ J Surg 2005; 75:936–9.
Anscher MS, Jones P, Prosnitz LR, et al. Local failure and margin status in early-stage breast carcinoma treated with conservation surgery and radiation therapy. Ann Surg 1993; 218:22–8.
Silverstein MJ, Lagios MD, Groshen S, et al. The influence of margin width on local control of ductal carcinoma in situ of the breast. N Engl J Med 1999; 340:1455–61.
Leong C, Boyages J, Jayasinghe UW, et al. Effect of margins on ipsilateral breast tumor recurrence after breast conservation therapy for lymph node-negative breast carcinoma. Cancer 2004; 100:1823–32.
Smitt MC, Horst K. Association of clinical and pathologic variables with lumpectomy surgical margin status after preoperative diagnosis or excisional biopsy of invasive breast cancer. Ann Surg Oncol 2007; 14:1040–4.
Dillon MF, Hill ADK, Quinn CM, et al. A pathologic assessment of adequate margin status in breast-conserving therapy. Ann Surg Oncol 2006; 13:333–9.
Aziz D, Rawlinson E, Narod SA, et al. The role of reexcision for positive margins in optimizing local disease control after breast-conserving surgery for cancer. Breast J 2006; 12:331–7.
Dzierzanowski M, Melville KA, Barnes PJ, et al. Ductal carcinoma in situ in core biopsies containing invasive breast cancer: correlation with extensive intraductal component and lumpectomy margins. J Surg Oncol 2005; 90:71–6.
Chagpar AB, Martin RCG 2nd, Hagendoorn LJ, et al. Lumpectomy margins are affected by tumor size and histologic subtype but not by biopsy technique. Am J Surg 2004; 188:399–402.
Miller AR, Brandao G, Prihoda TJ, et al. Positive margins following surgical resection of breast carcinoma: analysis of pathologic correlates. J Surg Oncol 2004; 86:134–40.
Mai KT, Chaudhuri M, Perkins DG, et al. Resection margin status in lumpectomy specimens for duct carcinoma of the breast: correlation with core biopsy and mammographic findings. J Surg Oncol 2001; 78:189–93.
Moore MM, Borossa G, Imbrie JZ, et al. Association of infiltrating lobular carcinoma with positive surgical margins after breast-conservation therapy. Ann Surg 2000; 231:877–82.
Taghian A, Mohiuddin M, Jagsi R, et al. Current perceptions regarding surgical margin status after breast-conserving therapy: results of a survey. Ann Surg 2005; 241:629–39.
Barlow WE, Lehman CD, Zheng YY, et al. Performance of diagnostic mammography for women with signs or symptoms of breast cancer. J Natl Cancer Inst 2002; 94:1151–9.
Barlow WE, White E, Ballard-Barbash R, et al. Prospective breast cancer risk prediction model for women undergoing screening mammography. J Natl Cancer Inst 2006; 98:1204–14.
Kuhl CK, Schrading S, Bieling HB, et al. MRI for diagnosis of pure ductal carcinoma in situ: a prospective observational study. Lancet 2007; 370:485–92.
Beatty JD, Porter BA. Contrast-enhanced breast magnetic resonance imaging: the surgical perspective. Am J Surg 2007; 193:600–5.
Deurloo EE, Peterse JL, Rutgers EJT, et al. Additional breast lesions in patients eligible for breast-conserving therapy by MRI: impact on preoperative management and potential benefit of computerised analysis. Eur J Cancer 2005; 41:1393–401.
Solin LJ, Orel SG, Hwang W-T, et al. Relationship of breast magnetic resonance imaging to outcome after breast-conservation treatment with radiation for women with early-stage invasive breast carcinoma or ductal carcinoma in situ. J Clin Oncol 2008; 26:386–91.
Menes TS, Tartter PI, Bleiweiss I, et al. The consequence of multiple re-excisions to obtain clear lumpectomy margins in breast cancer patients. Ann Surg Oncol 2005; 12:881–5.
O’Sullivan MJ, Li T, Freedman G, et al. The effect of multiple reexcisions on the risk of local recurrence after breast conserving surgery. Ann Surg Oncol 2007; 14:3133–40.
Cellini C, Hollenbeck ST, Christos P, et al. Factors associated with residual breast cancer after re-excision for close or positive margins. Ann Surg Oncol 2004; 11:915–20.
Darvishian F, Hajdu SI, DeRisi DC. Significance of linear extent of breast carcinoma at surgical margin. Ann Surg Oncol 2003; 10:48–51.
Ooi CWL, Serpell JW, Rodger A. Tumour involvement of the re-excision specimen following clear local excision of breast cancer with positive margins. ANZ J Surg 2003; 73:979–82.
Tartter PI, Bleiweiss IJ, Levchenko S. Factors associated with clear biopsy margins and clear reexcision margins in breast cancer specimens from candidates for breast conservation. J Am Coll Surg 1997; 185:268–73.
Jardines L, Fowble B, Schultz D, et al. Factors associated with a positive reexcision after excisional biopsy for invasive breast cancer. Surgery 1995; 118:803–9.
Kearney TJ, Morrow M. Effect of reexcision on the success of breast-conserving surgery. Ann Surg Oncol 1995; 2:303–7.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kurniawan, E.D., Wong, M.H., Windle, I. et al. Predictors of Surgical Margin Status in Breast-Conserving Surgery Within a Breast Screening Program. Ann Surg Oncol 15, 2542–2549 (2008). https://doi.org/10.1245/s10434-008-0054-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-008-0054-4